Premature Babies - A Success Story
One of the success stories in modern medicine has been the increasing survival of very premature babies. Over the past decade survival has improved dramatically for babies born at 26 weeks of gestation and above so that now over 80% survive.
Normal pregnancy lasts 40 weeks, but babies may survive from as early as 22 weeks, although at these extremely low gestations (22-24 weeks) many babies are born too immature to survive. As with all advances in care, there is a cost in terms of disability suffered by some children among those that survive.
This is the whole point of EPICure, as it allows us to quantify the outcomes and shows us where we need to target our care.
For parents faced with the prospect of delivering a child before 26 weeks of gestation, there has been little information available which describes the outcomes from large numbers of children. Thus, until we carried out the first study it had been difficult to give parents accurate information regarding the chances of survival and the possibility of disability or other long-term problems amongst survivors. Because care improves, and more babies survive, we hope outcomes also improve but we need to show this as well – hence we carried out EPICure2.
It is now over 15 years since we first studied the children that we included in EPICure2. Information is published frequently now about extremely low gestational ages and survival continues to improve at all gestations. Keeping up with this new knowledge is challenging and in some of the sections, we signpost where to go to for up-to-date information. Of course, the EPICure participants are continuing to get older and we will continue to study their very long-term outcomes for as long as we can. Few studies have made it to 19 years from around the world and the dedicated researchers who have done are coming together in important initiatives to share information on outcomes to increase our understanding further.
Why do we need to study extreme prematurity?
We know that disability increases as gestation at birth gets shorter. Births (and surviving children) at gestations below 27 weeks are relatively uncommon – being less than 1% of all births. Babies born this early need to stay in neonatal units for a long time and their care is very intense and costly. Because the number of extremely premature babies born is so small, we need large studies to be accurate in describing their outcomes.
The decision to admit a preterm baby for intensive care is made by doctors after discussion with the parents but until 2000 there were no national guidelines or data on which to build them. Data from EPICure have informed important national initiatives such as the report from the Nuffield Council on Bioethics describing many of the issues surrounding decision making in the period around birth (Nuffield Council Report). Some of these new guidelines – the latest published in 2019 - have been based on the results of the EPICure studies (BAPM Framework for Practice).
Data from the EPICure Studies have also influenced new national guidelines for the developmental follow-up of preterm babies after they leave neonatal care, published by NICE (the National Institute for Health and Care Excellence) in 2017 (NICE developmental follow-up of children and young people born preterm guideline).
The attitude of individual neonatologists and obstetricians may influence the management of different babies. The information on which that management is based needs to be impartial as possible as, on the basis of such decisions, treatments that are thought to be effective may be withheld. Clinicians, healthcare planners and parents need population-based data relevant to modern intensive care practices for informed decision making. EPICure has given them this nationally based information, which can be used to help this process.
Studying childhood outcomes for this group is important for everyone. Parents, doctors, teachers, health planners. Highlighting the chances of special needs for some extremely preterm children brings their upbringing into focus and emphasises where there are similarities and where there are differences from individuals who were not preterm. We have helped to develop support materials for teachers to assist in this which can be found here.
What are the EPICure studies?
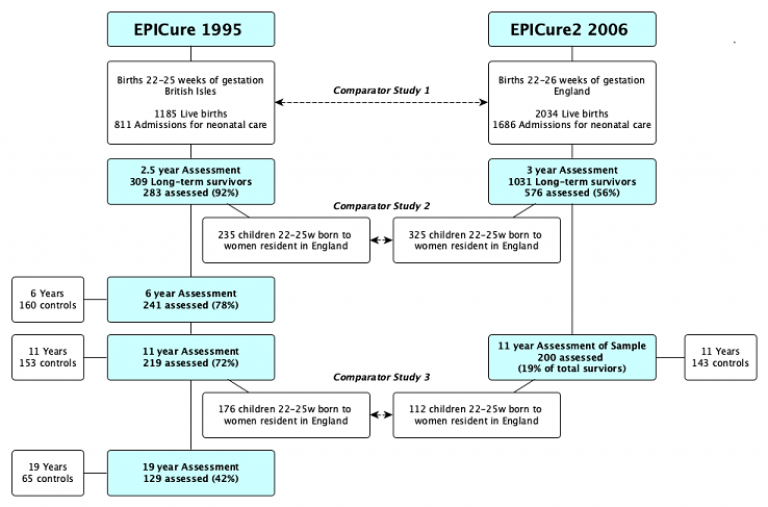
The EPICure studies comprise two birth cohorts of children born either in 1995 before 26 weeks of gestation or in 2006 before 27 weeks. There have been 5 main studies for the first and 3 for the second cohort as set out in the figure below.
What are we up to now?
We are continuing our analysis of the latest EPICure studies. Our current analyses include the eye outcomes we evaluated in EPICure@19 and the putting together the results of the important magnetic resonance scans we did with the other assessments we made. We are just analysing the EPICure2@11 study results and with these making important comparisons with the results of the previous cohort.
We have been working with the British Association of Perinatal Medicine (BAPM) to update our national guidance.
To ensure we maximise the use of the valuable information given to us by our participants and their families, we are working with researchers all over the world to compare and contrast outcomes is many different settings. Two important groups we are working with are:
The Adult Born Preterm International Collaboration (APIC). With this group we are studying mental health outcomes, blood pressure, growth and other aspects of young adult life after preterm birth.
The EU-funded RECAP-preterm Study is a similar collaboration covering all of our data. Having anonymised the dataset so that no one can be identified we are collaborating with the University of Warwick to set the data up so it can be used by any researcher together with Prof Marlow and his team. This will ensure we can use it to explore new ideas and draw new conclusions into the future.
We also offer the chance of using our data to explore new ideas by working directly with us – the EPICure data sharing agreement sets out how we do this.
 Close
Close

