Autosomal Recessive Bestrophinopathy (ARB) is the only bestrophinopathy to be recessive in its mode of inheritance.
What is Autosomal Recessive Bestrophinopathy (ARB)?
ARB was first described in 2008 and is the only bestrophinopathy to date which follows a recessive mode of inheritance, parents of affected individuals usually have normal vision. ARB is a rare disease, estimated to affect less than 1 in a million people. The onset of ARB can vary however, the majority of cases are diagnosed in the first two decades of life.
How does ARB affect the eye?
Patients with ARB tend to present to the clinic with central vision loss. Upon examination the fundus appears speckled, with irregularities of the RPE cells and the presence of yellow/white dots or flecks scattered across the retina, thought to be fatty deposits of lipofuscin. These small lesions can be detected due to their autofluorescence. Some patients with ARB can go on to develop cystoid macular edema (swelling caused by leaky blood vessels and fluid build-up under the retina). At later stages the presence of lesions and edema can lead to macular lesions, central scarring and extensive vision loss. The image below is a schematic for ARB:
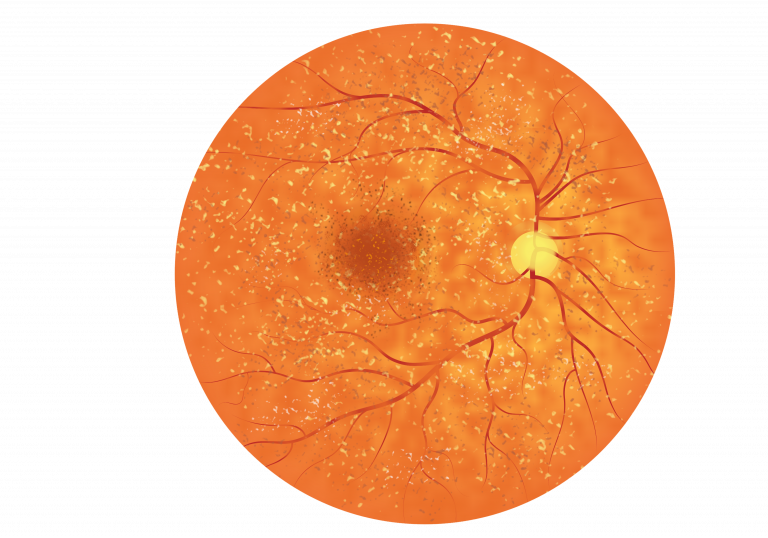
Patients with ARB can gradually progress from having 6/6 vision to having vision less than 6/60 on the Snellen chart, but if choroidal neovascularization (CNV) occurs then this could lead to a rapid deterioration in vision. Those with ARB also are more likely to suffer from hyperopia (being long-sighted).
Patients with ARB can also have changes at the front of the eye, affecting fluid flow in a region between the iris and cornea, known as the anterior chamber. Having a shallow anterior chamber can increase the pressure in the eye, putting patients at risk of developing glaucoma. If left untreated, glaucoma can damage the optic nerve, leading to blindness.
How is ARB diagnosed?
OCT imagery can be used to locate and measure the thickness and progression of the scattered lesions. OCT can also be used to image the build-up of fluid in ARB.
Autofluoresence imaging can also be used to examine small areas of hyperautofluorescence and hypoautofluorescence created by the small lesions and fluid accumulation beneath the retina.
Patients with ARB also have abnormal ERG and EOG recordings.
Diagnosis of ARB can be confirmed with genetic testing.
Are there any complications associated with ARB?
The main complication for ARB patients is the presence of choroidal neovascularization (CNV), where new blood vessels, originating from the choroid blood supply, grow towards the RPE and retinal cells. These new vessels are delicate and can easily rupture leading to fluid build-up within the retina. Fluid build-up can cause visual distortion or sudden loss of vision. Cystoid macula edema, swelling caused by fluid build-up, is also a complication of ARB which, if left untreated, can lead to vision loss.
Patients with ARB are more likely to suffer from hyperopia.
What are the treatment options for ARB?
There are currently no medical or surgical treatments available for ARB, or any of the bestrophinopathies, however research is ongoing and promising.
Some of the complications of ARB can be treated:
Choroidal Neovascularization (CNV)
Anti-VEGF injections can be injected into the eyes of patients in a hospital setting by doctors to stop the growth of new blood vessels, with the aim of preserving vision.
Macular Edema
The swelling causes by cystoid macular edema can be treated by injection of diuretics and steroids into the back of the eye.
Far-sightedness
Hyperopia (the ability to see objects at distance but close objects appear blurry) can be treated with prescription lenses and contact lenses.
Glaucoma
Patients at risk of glaucoma receive regular monitoring to check the pressure within the eye. Glaucoma can be treated using eye drops during the early stages, and with laser treatment or surgery in later stages.
Research into treatments for ARB is ongoing. Patients are encouraged to visit the many charities and support groups for bestrophinopathies.
 Close
Close

