Preclinical Neonatal Neuroprotection
The Group had its origins in the mid 1990s when, following the first acquisition of a phosphorus-31 spectrum from a preterm infant, Prof Reynolds (FRS) wished to study brain energy metabolism in a pre-clinical model. These experimental studies in the mid-1990s formed the scientific underpinnings for the translation of hypothermic (HT) neuroprotection from experimental studies to term neonatal encephalopathy (NE).
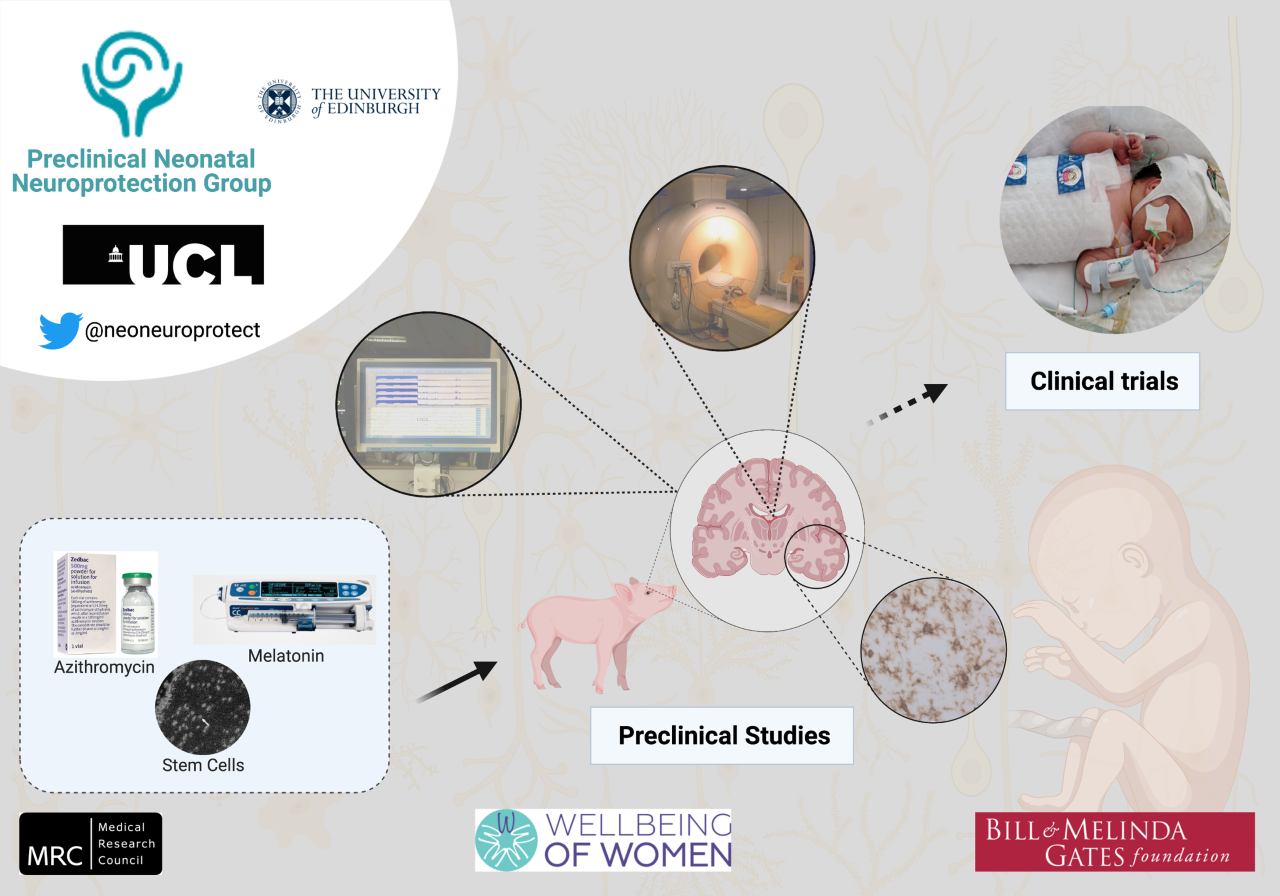
Professor Nicola Robertson joined UCL in 2003 to lead the Preclinical Neuroprotection Group. The group has grown considerably with international recognition of our unique preclinical model for NE. This model is highly clinically relevant; our animal intensive care unit utilises aEEG monitoring, servo-controlled cooling devices, invasive physiological monitoring, near infrared spectroscopy monitoring and 3-Tesla magnetic resonance imaging that are widely used in the neonatal intensive care setting. We aim to assess the safety and efficacy of neuroprotective therapies and translate the most promising to clinical trials to improve outcomes in babies with NE. Over the past 18 years, therapies investigated include: melatonin, magnesium sulphate, erythropoietin and more recently, human mesenchymal stem cells. In particularly, we have shown in several studies that intravenous, high dose melatonin is safe and augments therapeutic hypothermia in NE. Clinical trials are now urgently needed.
In 2021, Professor Nicola Robertson further expanded the group, establishing an additional laboratory based at the Roslin Institute and Large Animal Research and Imaging Facility (LARIF), University of Edinburgh. This partnership will provide the opportunity to establish a recovery model to assess neurodevelopmental outcomes. Together, we hope to accelerate the translation of new therapies from bench to bedside in the next 5-10 years.
 Close
Close