There are three major aims of the maternal medicine group.
- To understand the pathogenesis of gestational syndromes, in particular pre-eclampsia and acute fatty liver of pregnancy. Our goal is to understand the pathology of these multi-system disorders in order to better identify women at risk and implement targeted prophylaxis and treatment, to improve pregnancy outcome for mother and infant.
- To investigate whether acquired parental traits, specifically obesity, is inherited by their children through epigenetic mechanisms.
- To investigate whether a parental genotype predisposes to fetal growth restriction at high altitude in India.

Dr David Williams PhD FRCP
Research Group Lead
Group members
- Dr David Williams PhD, FRCP Honorary Senior Lecturer, Maternal Medicine.
- Dr Sara Hillman PhD, MRCOG Lecturer, Maternal and Fetal Medicine
- Agata Ledwozyw, PhD student, UCL
- Dr Mandeep Kaler MRCOG, clinical PhD student, UCL
- Dr Fredrika Asenius, clinical PhD student, UCL
- Dr Tamara Kubba, clinical research fellow
- Dr Alice Hurrell, entry level scholar, Wellbeing of Women
- Dr Elena Mantovani, Maternal and Fetal Medicine fellow
Collaborators
- Professor Vardhman Rakyan, Epigenetics, Blizard Institute, Queen Mary University London (QMUL)
- Professor Rachel Batterham, Diabetes, Endocrinology and Obesity, UCL
- Professor Juan-Pablo Casas, Farr Institute, UCL
- Professor Raymond MacAllister, Clinical Pharmacology, UCL.
- Professor Aroon Hingorani, Genetic Epidemiology, Institute of Cardiovascular Science, UCL
- Professor Asif Ahmed, Vascular Biology, Aston University
- Dr Michelle Holland, Epigenetics, Blizard Institute, QMUL
- Dr Philip Hennis, Institute for Sports, Exercise and Health, UCL
- Dr Hywel Williams, GOSgene, UCL Institute for Child Health
- Dr Chiara Bacchelli, Principal Research Associate, in Personalised Medicine, UCL Institute for Child Health
- Dr Mohammad Ibrahim (Clinical Immunology, Kings College)
- Dr Muna Noori, Consultant Obstetrician, Queen Charlotte’s Hospital, London
- Dr Leanne Bellamy, GP, Torquay
Current Maternal Medicine PHD projects
- 2012 - 2016 Agata Ledwozyw: A study of maternal immune changes before and during pre-eclampsia. In collaboration with Professor Lucy Clapp in Clinical Pharmacology.
- 2013 - 2017 Mandeep Kaler: A study into the pathogenesis of acute fatty liver of pregnancy (Mandeep Kaler). In collaboration with Dr Ross Breckenridge, Clinical Pharmacology, UCL and Dr Phil Hennes, Institute of Sports, Exercise and Health, UCL.
- 2015 - Fredrika Asenius: Inheritance of Epigenetic marks from father to offspring (Fredrika Asenius). In collaboration with Professor Vardhman Rakyan, Epigenetics, Blizzard Institute, Queen Mary University London.
PHD studentships awarded
2014: Dr Sara Hillman PhD: The Role of Genetics and Environment on Fetal Growth, UCL
2010: Dr Muna Noori PhD: Maternal circulating and vascular factors in Pre-eclampsia
2006: Dr Veronique Bachy PhD: The role of Maternal Innate Immunity in healthy pregnancy and pre-eclampsia
Current clinical trials
The Stamp Trial: a multi-centre double-blind, placebo-controlled trial of Pravastatin to ameliorate early severe pre-eclampsia, in collaboration with Aston and Birmingham Universities. Publication of this Medical Research Council (MRC) funded, UCL-sponsored trial is expected in 2016.
An investigation into the genetics of fetal growth restriction in India. Dr Sara Hillman has been awarded a seed fund grant from The Wellcome Trust (£100,000) to investigate the genetics of fetal growth in collaboration with the All India Institute of Medical Sciences (AIIMS), Delhi and Sonam Norbu Memorial Hospital, Leh, India.
Pre-eclampsia research
Background to Pre-eclampsia Research
Pre-eclampsia is a multi-system syndrome of pregnancy characterized by gestational hypertension and proteinuria. Pre-eclampsia affects 3-5% of pregnancies and worldwide is associated with over 60,000 maternal deaths per year. Delivery remains the only cure, but premature delivery can be detrimental to neonatal health whilst delayed delivery exposes the mother to the escalating risks of an unpredictable multi-system disorder.
Utero-placental pathology from pregnancies affected by pre-term pre-eclampsia is similar to that found in pregnancies affected by fetal growth restriction (FGR). Late pre-eclampsia is often associated with a relatively large placenta and normal sized babies. Inadequate placental invasion and incomplete adaptation of maternal spiral arteries in early pregnancy, leads to placental ischaemia, reduced fetal growth and in vulnerable women to pre-eclampsia.
The mechanism by which the placenta invades the uterine placental bed and induces angiogenesis involves a delicately regulated interaction of immunological and angiogenic factors. Placental derived growth factors involved in placental angiogenesis have altered expression in pre-eclampsia and fetal growth restriction, which are also involved in cardiovascular disease.
Agata Ledwozyw is investigating the relationship between maternal immunosuppressive factors and placental angiogenic factors in women at risk of pre-eclampsia.
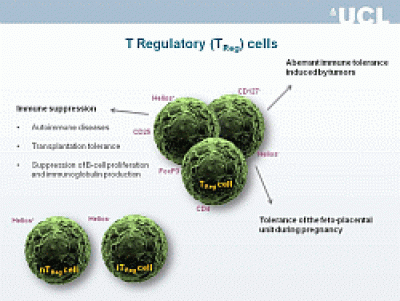
Current Projects in Pre-eclampsia
Acute fatty liver of pregnancy
Acute Fatty Liver of Pregnancy (AFLP) affects approximately 1:10,000 pregnancies, but it is a devastating syndrome that causes death and profound disability of mother and newborn. AFLP resembles a fatty acid oxidation (FAO) defect. However, two FAO enzyme deficiencies associated with the condition do not explain the majority of cases.
Dr Mandeep Kaler is investigating the cause of AFLP in previously affected families using novel techniques to identify functional defects in FAO. She is using whole genome sequencing to identify novel gene variants associated with fatty acid metabolism. Identification and treatment of novel metabolic disorders could prevent the disorder in the first place and reduce on going morbidity in affected offspring.

Pregnancy: a predictor for future health
During pregnancy, almost every organ of the mother's body has to work harder in order to meet the demands of the developing fetus. Women with chronic disease struggle to fulfil these physiological demands. As a consequence, pregnancy outcome can be compromised and long-term maternal health may be threatened.
Gestational syndromes generally develop in the second half of pregnancy when the physiological burden of pregnancy is at its greatest. For example, the progressive insulin resistance of pregnancy acts as a stress-test that transiently unmasks carbohydrate intolerance which we term “gestational diabetes mellitus” in women who are predisposed to type-2 diabetes. Childbirth leads to remission of the maternal condition, but the disease returns in later life when the effects of aging and weight gain expose a persistent vulnerability to diabetes.
Currently, we are investigating the consequences of acute fatty liver of pregnancy on future maternal health.
Intergenerational Inheritance Of Epigenetic Marks From Obese Father To Growth Restricted Offspring
We have shown that obese men with insulin-resistance are at risk of fathering growth-restricted babies with epigenetic changes to metabolism-controlling genes.(Hillman S. et al. Diabetes Care 2013;36:1675-1680 and Hillman SL. et al. Epigenetics 2015;10:50-61)
In collaboration with Professor Vardhman Rakyan’s group at QMUL, we are investigating whether there is evidence of intergenerational inheritance of acquired epigenetic marks from obese fathers to growth-restricted babies. Further, could pre-conception paternal weight loss reverse obesity-related DNA methylation profiles (DMPs)?
Key research funding
- 2015-2016: NIHR UCLH BRC & UCLH Charitable Trustees/Clinical Research and Development Committee (CRDC) (£39,855). The effect of paternal obesity and weight loss on sperm DNA methylation profiles and the potential for intergenerational inheritance of epigenetic marks.
- 2015-2018: Rosetrees Trust PhD studentship for Fredrika Asenius (£60,000). Paternal Health and Pregnancy Outcome; an investigation into the role of paternal insulin resistance and weight loss on fetal growth and development.
- 2015: Wellbeing of Women, Entry Level Scholarship (ELS409) for Alice Hurrell (£19,998). Vasoactivity and Autoimmunity in Pre-eclampsia.
- 2014: Elizabeth Garrett Anderson Trustees (£24,500). To investigate the role of angiotensin II autoantibodies in the pathogenesis of pre-eclampsia.
- 2013: Elizabeth Garrett Anderson Trustees (£21,641).An investigation into the circulating and maternal vascular factors that mediate vasoconstriction during the pregnancy-syndrome pre-eclampsia.
- 2012-2015: UCL Impact Studentship with GlaxoSmithKline and Alere for Agata Ledwozyw (£65,070)An investigation into the circulating and maternal vascular factors that mediate vasoconstriction during the pregnancy-syndrome pre-eclampsia.
- 2010-2013: Wellbeing of Women Clinical Research Fellowship for Dr Sara Hillman (£174,000);An investigation of parental phenotype and epigenetic changes associated with pregnancies affected by fetal growth restriction.
- 2010 -2015: BMA Joan Dawkins Award 2010; (£55,000);An investigation of epigenetic changes to insulin control genes in fathers and offspring of pregnancies affected by fetal growth restriction.
- 2009: UCL/UCLH CRDC Starter Grant (£78,950) CRDC Fast-Track funding (£27,500):An investigation into insulin resistance of men who father pregnancies complicated by pre-eclampsia and fetal growth restriction
- 2010-11: A proof of principle randomised placebo-controlled trial for use of statins to ameliorate early onset preeclampsia (2008-11) With Birmingham UniversityMRC; £499753
- 2008-10: Paternal phenotype of fathers of pre-eclamptic and fetal growth restricted pregnancies. UCLH/UCL CBRC. £78,000 and for equipment from EGA Trustees, £25,500 and UCL/UCLH CDRC, £26,000
 Close
Close

