International trial finds better treatment for people with drug-resistant tuberculosis
22 December 2022
A new all-oral, shorter treatment regimen for drug-resistant tuberculosis (TB) is safer and more effective than current options for people with drug resistant TB, according to results from a global trial featuring UCL researchers.
The study, published by The New England Journal of Medicine, tested three novel combinations of TB treatments taken orally over six months against the accepted standard of care. All were shown to be more effective - with fewer side effects - than the current nine-month regimen that is used to treat drug-resistant TB.
The findings are the results from the TB-PRACTECAL trial - the first-ever multi-country, randomised, controlled clinical trial to report on the efficacy and safety of a six-month, all-oral treatment regimen. Coordinated by Medicine Sans Frontiers (MSF), the TB-PRACTECAL trial involved 552 patients in seven sites across Belarus, South Africa, and Uzbekistan.
Study collaborator Tim McHugh, Professor of Medical Microbiology at UCL and lead of the microbiology and lab-testing components of the trial said: “Standard treatment for TB normally requires four drugs in six months and the drugs aren't very pleasant to take. But in many cases that treatment is successful. However, in an increasing number of cases, we're seeing the emergence of drug-resistant TB. The established treatments for drug-resistant TB are longer (routinely nine months) and the drugs are worse in their side-effects due to increased toxicity.”
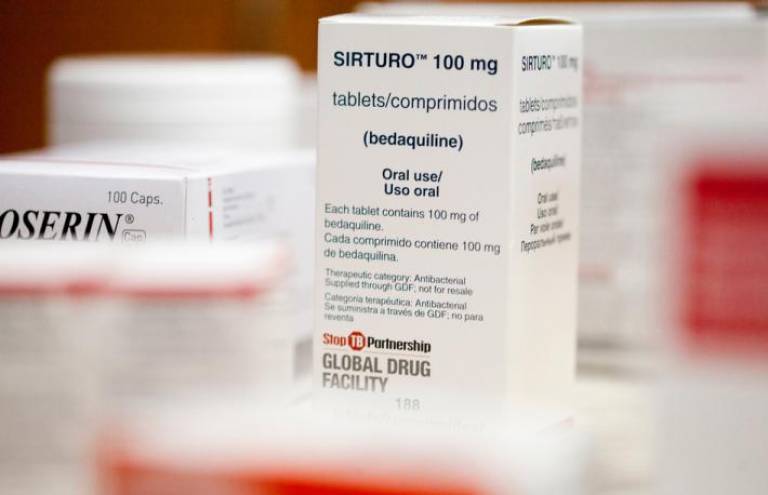
The TB-PRACTECAL trial found that a six-month regimen using the TB drugs bedaquiline, pretomanid, linezolid, and moxifloxacin (BPaLM) proved most effective and safe. The trial also studied a bedaquiline, pretomanid, and linezolid (BPaL) regimen; and a bedaquiline, pretomanid, linezolid, and clofazimine (BPaLC) regimen. All of which performed significantly better than the standard of care.
“We began the TB-PRACTECAL clinical trial nine years ago because something had to be done,” said Bern-Thomas Nyang’wa, MSF medical director and chief investigator of the trial. “Patients were telling us that the previous regimens were lengthy, ineffective, and grueling and that the side effects were worse than the disease itself. They also weren’t very effective; just one in two people were cured. The new regimen, BPaLM, has an 89 percent cure rate, is safer, shorter, and more tolerable with fewer pills.”
The results from the TB-PRACTICAL study, together with results from a linked study (ZeNix)* published in the New England Journal of Medicine, have prompted the World Health Organization (WHO) to update global drug-resistant TB treatment guidelines.
“The impact of these two studies is significant - the main outcome, for me, is the fact that these two trials have changed WHO guidance and clinical practice, with safer more effective treatment options now available for TB patients,” said Professor McHugh who together with Prof Angela Crook, Medical Statistician MRC Clinican Trials Unit at UCL, was a key collaborator on ZeNix.
For the UCL research team, the next phase of the TB-PRACTICAL study will be to work with trial collaborators in Uzbekistan in using whole genome sequencing analysis to extract further information from the data obtained.
* Bedaquiline–Pretomanid–Linezolid Regimens for Drug-Resistant Tuberculosis. ZeNix clinical trial results. New England Journal of Medicine, September 2022
Further information
- Professor Tim McHugh academic profile
- Professor Angela Crook academic profile
- TB-PRACTICAL trial: A 24-Week, All-Oral Regimen for Rifampin-Resistant Tuberculosis. NEJM. December 2022
- UCL-TB News: ZeNix trial success announced
- UCL News: Shorter treatment effective for drug-resistant tuberculosis STREAM clinical trial
- UCL Division of Infection and Immunity
- The Medical Research Council Clinical Trials Unit (MRC CTU) at UCL
- UCL TB network
- WHO consolidated guidelines on tuberculosis. Module 4: treatment - drug-resistant tuberculosis treatment, 2022 update
- Medicins Sans Frontieres
- Photo: EndTb.org
 Close
Close

