To learn more about the study and the study team, please click on the relevant section below.
- About the study
There are many disease modifying treatments (DMTs) for patients with Multiple Sclerosis (MS). Currently, there is no clinical tool to help patients select the medication that will work best for them and the decision is often made according to factors such as drug administration, frequency of drug administration and risk of side effects. If patients continue to suffer from relapses or have serious side effects, they can switch to another DMT. The consequences of this policy that requires a DMT to “fail” before prescribing another one include continuous relapses, accumulation of disability and unnecessary side effects.
We aim to collect all manifestations of MS that may influence individual treatment response and translate machine learning techniques into clinical practice in order to generate a tool which will predict treatment response, thereby guiding the choice of DMT and reducing the risk of adverse events given by unnecessary treatments.
- Study Schedule
This is an observational study, where patients with MS initiating a DMT in the NHS will undergo clinical and MRI assessments and blood tests. We will recruit adult patients and children with MS from the MS clinics at UCLH and the UK Paediatric Neuroinflammation Services (Great Ormond Street Hospital, Evelina Children’s Hospital London and Birmingham Women & Children’s Hospital).
Participants will be seen at three timepoints: baseline, 6 months and 18 months. At each visit they will undergo a standardised clinical assessment, blood tests for neurofilaments levels, safety data and MRI scans.
Clinical Assessment
The clinical assessment will comprise scales for physical disability, such as the EDSS, and the Brief International Cognitive Assessment for MS (BICAMS). Participants will also be asked to complete some patient reported outcome measures (PROMs), as well as providing information on their medical history, demographics, comorbidities, diet, education and employment.
- Magnetic Resonance Imaging (MRI)
MRI will include standard-of-care protocols, which include 3D-FLAIR and T2-TSE axial imaging and research sequences such as a volumetric brain sequence (3D-T1).
- Genetics
Genetic factors may enable us to identify patients who are at higher risk of accumulation of brain pathology.
The genetic testing will identify those variants previously associated with MS susceptibility and will be undertaken at the UCL Institute of Neurology by Professor Henry Houlden, Professor of Neurogenetics, and his team.
- Neurofilaments in Serum
Neurofilament levels in serum act as a blood biomarker of axonal damage, allowing for reliable, clinical monitoring of axonal damage in MS patients. They will be measured at each time point.
The concentration of neurofilaments in serum will be determined at the UCL Institute of Neurology by Professor Henrik Zetterberg, Professor of Neurochemistry, and his team, with the neurofilament-light assay.
- Machine Learning
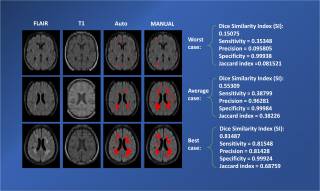
Machine learning will be employed to segment MS lesions. Additionally, high-dimensional models will be constructed to predict individual treatment response, using all the characteristics that define the disease in an individual.
A positive treatment response will be defined as no evidence of disease activity or NEDA (no relapses, no progression of disability and no MRI activity. All predictions will be probabilistic. The high-dimensional models will be constructed in a tiered approach and the most parsimonious, efficient, predictive model will be created. Overfitting will be minimised and model training, validation and testing using external datasets will be performed.
- PITMS Research Team & Partners
UCL and UCLH
Professor Olga Ciccarelli, Principal Investigator
Dr Yael Hacohen, Co-Investigator
Professor Parashkev Nachev, Co-Investigator
Professor Daniel Alexander, Co-Investigator
Professor Henry Houlden, Co-Investigator
Professor Henrik Zetterberg, Co-Investigator
Dr Sarmad Al-Araji, Clinical Research Fellow (2019 - 2022)
Dr Alessia Bianchi, Clinical Research Fellow
Alvin Zapata, Research Nurse
Dr Le Zhang, Research Associate – Computational Imaging (2019 - 2022)
Dr Baris Kanber, Senior Research Fellow – Machine Learning
Amber Strang, Study Coordinator
Great Ormond Street Hospital
Dr Cheryl Hemingway, Site Principal Investigator
Dr Omar Abdel-Mannan, Clinical Research Fellow
Katie Hanson, Clinical Nurse Specialist
Evelina Children’s Hospital
Dr Ming Lim, Site Principal Investigator
Birmingham Women’s & Children’s Hospital
Dr Evangeline Wassmer, Site Principal Investigator
- Publications
Abdel-Mannan O, and the UK-Childhood Inflammatory Disease Network. Use of Disease-Modifying Therapies in Pediatric Relapsing-Remitting Multiple Sclerosis in the United Kingdom. Neurol Neuroimmunol Neuroinflamm. 2021 May 21;8(4):e1008. doi: 10.1212/NXI.0000000000001008.
Al-Araji S, Bianchi A, Eshaghi A, et al, …Ciccarelli O. Assessing predictors of NEDA in RRMS patients initiating dimethyl fumarate in a real-world setting. P113. Association of British Neurologists (ABN) 2022.
Al-Araji S, Jha A, Zhang L, et al, …Ciccarelli O. Bayesian prediction of individualised treatment response in multiple sclerosis. ECTRIMS October 2022. Selected for poster award.
Moccia M, Al-Araji, Zhang L, et al…, Ciccarelli O. Comparing clinical and radiological effectiveness of disease modifying treatments in the real-world. O955. ECTRIMS October 2022.
Eshaghi A, Young AL, Wijeratne PA, et al…, Ciccarelli O. Identifying multiple sclerosis subtypes using unsupervised machine learning and MRI data. Nat Commun. 2021 Apr 6;12(1):2078. doi: 10.1038/s41467-021-22265-2. (*)
Eshaghi A, Wijeratne P, Oxtoby N, et al…, Ciccarelli O. Predicting personalized risk of disability worsening in multiple sclerosis with machine learning. Nat Commun. 2022. Major revisions requested. (*)
Zhang L, Tanno R, Bronik K, et al. Ciccarelli O, Alexander DC. "Learning to segment when experts disagree." International Conference on Medical Image Computing and Computer-Assisted Intervention, pp. 179-190. Springer, Cham, 2020.
Zhang L, Tanno, R Xu MG, Ciccarelli O, Barkhof F, Alexander DC. "Disentangling Human Error from the Ground Truth in Segmentation of Medical Images." 34th Conference on Neural Information Processing Systems (NeurIPS 2020).
- Contact Us
(07976) 846695
 Close
Close





