MDC Publication Highlights - May 2020
8 June 2020
Understanding the experiences of people with late stage Parkinson's, Untangling the roles of GCase and alpha-synuclein in the progression of Parkinson’s pathology & Unraveling the enigma of cortical tremor
Understanding the experiences of people with late stage Parkinson's
There is a surprising scarcity of research into of the problems encountered by people in the late stages of Parkinson’s disease, even though this population experiences the greatest Parkinson’s-related impairment and requires significant medical and non-medical management. The Care of Late Stage Parkinsonism (CLaSP) study, led by Prof. Anette Schrag from UCL’s Queen Square MDC, is a longitudinal study of patients with late stage Parkinsonism across six major European health care systems. The study collected comprehensive information about motor and non-motor clinical features of people who have been diagnosed with Parkinson’s for seven years or more and are clinically determined to have advanced disease and/or significant disability. The 700 people who participated in the study were around 76 years of age and had an average disease duration of more than 15 years. As expected, the study found that severity and frequency of motor and non-motor symptoms was generally high in this patient population, higher that observed in early disease stages, but also higher than observed in people with advanced but not late stage Parkinson’s. One exception to this was severe dyskinesia leading to advanced therapies, which was quite rarely observed among the study’s cohort. The most common and disabling problems reported by people with late stage Parkinson’s were falls, severe motor symptoms with prolonged off-periods despite the large variety of available treatment option and the presence of hallucinations or delusions. These findings indicate that current treatment of late stage parkinsonism in the community remains insufficiently effective to alleviate disabling symptoms in many patients. The information collect through this study can be used to inform how best to provide effective care for this severely affected patient group and contribute to improved practices for clinical care.
Schrag et al. ‘The late stage of Parkinson's – results of a large multinational study on motor and non-motor complications’. Parkinsonism & Related Disorders, First Published: 21 May 2020, DOI: 10.1016/j.parkreldis.2020.05.016.
Untangling the roles of GCase and alpha-synuclein in the progression of Parkinson’s pathology
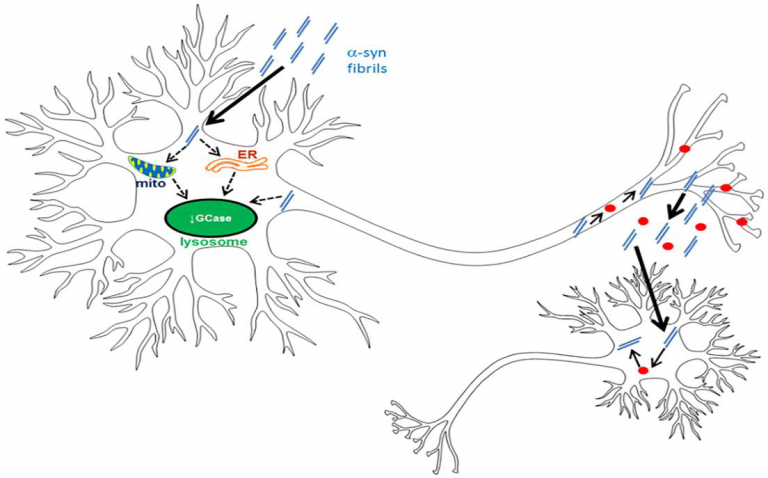
Mutations in the GBA gene, which cause reduced activity of a protein called GCase (glucocerebrosidase) are one of the most common genetic risk factors for Parkinson’s. Mutations in this gene disrupt the process of eliminating intra-cellular waste (through lysosomal autophagy), and importantly, disruptions in this cellular pathway are also seen in people with Parkinson’s who do not carry the gene mutation (so called “sporadic” Parkinson’s). Reduced GCase activity was shown to result in increased levels of alpha-synuclein, the protein which accumulates to form tangled masses that are considered the pathological hallmark of Parkinson’s disease. The current study, led by MDC researcher Prof. Tony Schapira, sought to understand the relationship between GCase activity and alpha-synuclein accumulation and how their interactions promote the Parkinson’s disease pathology. The researchers treated brain cells with preformed alpha-synuclein aggregates and examined their effects. They found that alpha-synuclein aggregates impaired GCase activity and also induced normal alpha-synuclein present in cells to take on an abnormal form more prone to aggregation. The researchers also found that cells in which GCase activity was inhibited released more aggregated alpha-synuclein into their surroundings and were thus more likely to “infect” other cells. This study sheds new light on the interactions between these two proteins and how they contributes to the pathology of Parkinson’s disease, suggesting that reduced GCase activity plays a key role in the spread of alpha-synuclein and thus influences the rate of disease progression.
Gegg M.E., Verona G. & Schapira A.H.V. ‘Glucocerebrosidase deficiency promotes release of α-synuclein fibrils from cultured neurons’. Human Molecular Genetics, First Published: 11 May 2020, DOI: 10.1093/hmg/ddaa085.
Unravelling the enigma of cortical tremor
Cortical tremor is a relatively recently described form of movement disorder. The disorder is familial, but the genes that cause it have not been fully identified yet. Its main characteristic is a tremor present during posture and action (but not at rest), most often in the hands, but which can also involve other parts of the body. Other clinical features common in families with cortical tremor include epilepsy and cognitive impairment. In this review, MDC researchers led by Prof. Kailash Bhatia present the clinical and genetic features of cortical tremor along with pathophysiological findings and suggest potential neural mechanisms underlying this disorder. The authors show that the core feature of cortical tremor is its rhythmicity and provide evidence suggesting that this can be driven by a cerebello-thalamo-cortical feedback loop. They propose that the cerebellum likely plays a major role in cortical tremor and could represent the link between this disorder and the wider spectrum of cortical myoclonus disorders.
Latorre et al. ‘Unravelling the enigma of cortical tremor and other forms of cortical myoclonus’. Brain, First Published: 17 May 2020, DOI: 10.1093/brain/awaa129.
 Close
Close

