Simple eye tests to predict Parkinson’s-linked dementia
5 December 2019
Quick and easy eye tests may predict which people with Parkinson’s disease are likely to develop dementia, finds a new study led by UCL Queen Square Institute of Neurology.
The tests, including commonly used eye charts and skewed images of cats and dogs, pick up warning signs in people who aren’t yet aware of any changes to their vision, according to the findings published in Neurology Clinical Practice. Researchers say being able to predict Parkinson’s dementia early could help with clinical trials, and the tests could also help track the disease’s progression, helping lead to more effective treatments in the future.
“It appears that Parkinson’s disease affects not only the brain, but the eyes as well, which could provide new insights into how the disease develops,” said lead author Dr Rimona Weil (Department of Neurodegenerative Disease, UCL Queen Square Institute of Neurology). “As we still don’t have a full understanding of how Parkinson’s disease works, our findings suggest the disease may have a more widespread effect than previously believed.”
Dementia is a common, debilitating aspect of Parkinson’s disease that affects 50% of people within 10 years of a Parkinson’s diagnosis. For the study, the researchers conducted visual, cognitive and motor tests on 146 people (112 with Parkinson’s and 34 healthy control subjects), in addition to ophthalmic examination and retinal imaging. They compared the visual measures to a risk score for Parkinson’s dementia, a recently developed algorithm validated in a longitudinal study that combines age of onset, gender, motor, mood and cognitive scores (the research team also validated the results by finding similar trends when using different risk algorithms in the analysis).
The eye tests that predicted an increased risk of dementia included a standard measure of visual acuity (the LogMAR chart), a colour vision test, and a measure of contrast sensitivity (Pelli-Robson chart) testing whether people can see faded grey letters on a white background. Recognition of biological motion was also impaired in those at higher risk of dementia, as shown by a test where participants had to identify a person walking from a series of moving dots.
Another relevant measure, the Cats-and-Dogs test, asking whether a distorted image shows a cat or a dog, was recently developed by Dr Weil and colleagues who had noticed that many people with Parkinson’s report difficultly in reading ‘CAPTCHA’ images used as online anti-robot measures. A study earlier this year found that poor performance in the Cats-and-Dogs test predicted worsening of Parkinson’s symptoms after a year-long follow-up.*
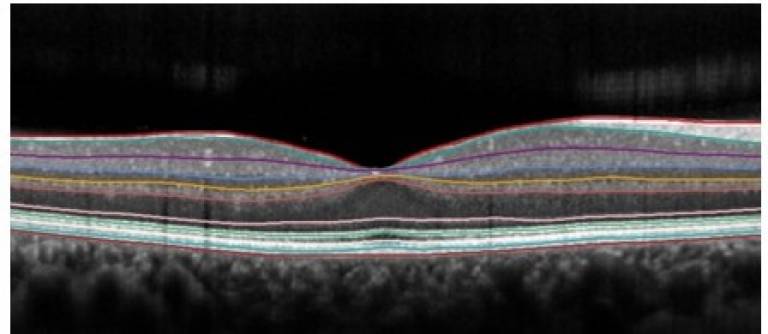
People at higher risk of Parkinson’s dementia also showed more retinal thinning, as shown in OCT (optical coherence tomography) scans, in parts of the retina that contain dopamine receptors, consistent with increasing evidence that Parkinson’s affects the retina.
The research is supported by other recent findings also led by Dr Weil identifying the brain networks involved in the early stages of Parkinson’s dementia, which could inform potential brain scans to predict who will develop dementia, as part of a larger set of tests.**
The study’s first author, Dr Louise-Ann Leyland (Department of Neurodegenerative Disease, UCL Queen Square Institute of Neurology), said: “We hope that our research can lead to the development of a suite of measures to identify candidates for clinical trials of potential Parkinson’s treatments, and to track disease progression. And hopefully in the future, if effective treatments for Parkinson’s dementia are developed, then these tests could identify who may benefit most from specific treatments.”
Dr Weil added: “There’s no indication that people with Parkinson’s should be concerned if they start to notice changes in their vision, as our study was picking up warning signs in people who were not aware of any problems with their vision. We’re not aware of any relationship between Parkinson’s dementia and common age-related vision problems such as cataracts or glaucoma.”
The researchers are continuing the study by following up a cohort of people with Parkinson’s disease to validate whether the eye tests do effectively predict the development of dementia.
The study involved researchers from UCL Queen Square Institute of Neurology, UCL Institute of Ophthalmology, UCLH, Lyon Neuroscience Research Center, University of California, San Diego, and Moorfields Eye Hospital, and was funded by the National Institute for Health Research (NIHR) UCLH Biomedical Research Centre, NIHR, Fight for Sight and Wellcome.
Professor David Dexter, Deputy Director of Research at Parkinson's UK, which supported in recruitment for the study, said: "Parkinson's is incredibly complex and unpredictable, but these visual tests show tremendous promise to help us identify dementia risks at an early stage. Unfortunately, dementia affects many people with Parkinson's at some point and has a devastating impact on individuals and their loved ones.
"The structural changes in the eye and changes in vision observed in this study highlights the potential of such tests to identify people at risk of developing dementia, which could ultimately help with the urgent need to provide better treatments and care, to help everyone affected by Parkinson's dementia.”
Further information
- Louise-Ann Leyland, Fion D. Bremner, Ribeya Mahmood, Sam Hewitt, Marion Durteste, Molly R.E. Cartlidge, Michelle M.-M. Lai, Luke E. Miller, Ayse P. Saygin, Pearse A. Keane, Anette E Schrag, & Rimona S. Weil, ‘Visual tests predict dementia risk in Parkinson’s disease’
- Dr Rimona Weil's academic profile
- Dr Louise-Ann Leyland's academic profile
* Weil et al (2019) Neural correlates of early cognitive dysfunction in Parkinson's disease. Annals of Clinical and Translational Neurology 2019; 6(5): 902–912 doi: 10.1002/acn3.767
** Rimona S Weil, Joey K Hsu, Ryan R Darby, Louis Soussand, Michael D Fox, Neuroimaging in Parkinson’s disease dementia: connecting the dots, Brain Communications, Volume 1, Issue 1, 2019, fcz006, https://doi.org/10.1093/braincomms/fcz006
Image: Relationship between the retinal volume and risk of Parkinson disease (PD) dementia
 Close
Close

