What is dementia?
Dr Jonathan Rohrer, Consultant Neurologist, Dementia Research Centre, UCL Institute of Neurology
“Dementia” is a term for progressive problems in thinking or behaviour – this may be:
- Memory, the main problem in Alzheimer’s disease
- Behaviour, the main problem in frontotemporal dementia
- Language, the main problem in semantic dementia and progressive non-fluent aphasia
Or other things, such as arithmetic, planning and problem solving
Different problems are seen in different dementias – some dementias affect the whole brain, such as Alzheimer’s disease, whereas others appear to affect only parts of the brain, for example the area for speech production in progressive non-fluent aphasia.
The most common form of dementia is Alzheimer’s disease and this accounts for about 60-70% of all cases. Vascular dementia caused by damage to the blood vessels in the brain is probably the next most common cause. The 3rd and 4th most common causes are frontotemporal dementia (which includes behavioural variant frontotemporal dementia and primary progressive aphasia) and Dementia with Lewy bodies. In total these four causes account for about 95% of all cases of dementia. There are many rare causes of dementia and these account for the final 5% of cases.
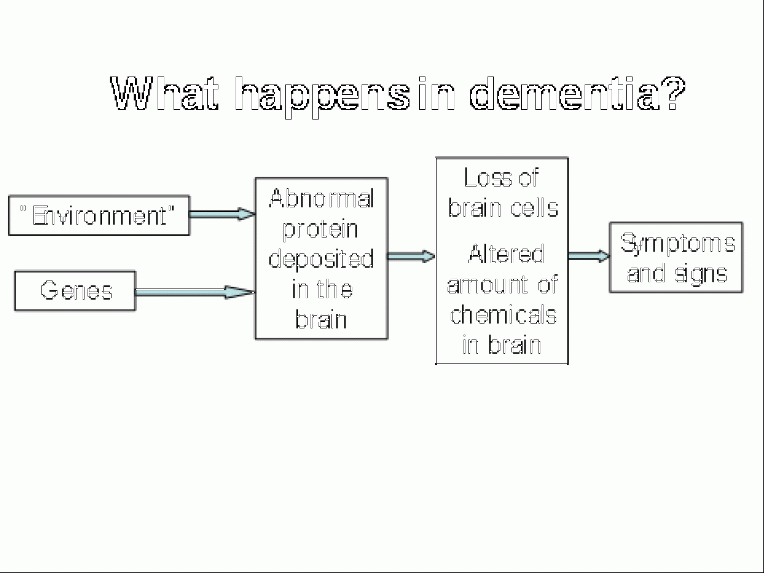
The diagram above is a simplistic way of thinking about what is happening in people’s brains as they develop dementia:
- For some people an abnormal gene triggers the disease (See the section “Is dementia inherited?” for more information). This is the case in up to 50% of people with frontotemporal dementia but only a very small amount of people with Alzheimer’s disease.
- However, for the people who do not have an abnormal gene a mixture of things probably trigger the disease – a mix of something from the “environment” and other genes. We currently know very little about what the triggers in the “environment” are but these are likely to include problems such as high blood pressure and diabetes.
- Once the disease is triggered, abnormal proteins become deposited in the brain. In frontotemporal dementia, these are proteins known as tau, TDP-43 and FUS, in Alzheimer’s disease it is tau and amyloid and in dementia with Lewy bodies it is something called alpha-synuclein.
- These abnormal proteins cause brain cells to die, and so brain cells from certain areas of the brain are slowly lost. In frontotemporal dementia the cells are lost from the frontal and temporal lobes of the brain while in Alzheimer’s disease cells are lost from the whole brain.
- Once cells are lost, the amount of chemicals in the brain becomes lower. Brain chemicals or “transmitters” are needed for signals to pass from brain cell to another. For example, in Alzheimer’s disease there is less of a chemical called acetylcholine. The aim of drugs such as donepezil (ARICEPT), rivastigmine (EXELON) and galantamine (REMINYL) is to try to increase the amount of this.
- Loss of cells and decreased amount of chemicals cause the symptoms and signs of the disease, which are different in different types of dementia.
Research in dementia takes place all over the world and more and more is becoming known about each of the different types of dementia. As our knowledge continues to increase, the hope is that we will be able to design treatments that will help combat the symptoms and signs of dementia, and eventually hopefully cure it.
What is Frontotemporal dementia (Pick's Disease)?
Dr Jonathan Rohrer & Dr Jason Warren, Dementia Research Centre
Frontotemporal dementia (FTD) is a group of conditions caused by loss of cells mainly in the frontal and temporal lobes of the brain. The main symptoms are a progressive change in personality and behaviour or progressive deterioration in language abilities.
It can affect both men and women and usually starts in the 40’s, 50’s or 60’s. However it can also affect older people, and rarely, even younger people.
It was originally described by Arnold Pick in 1892 after whom it was named. Most doctors now prefer to reserve the name ‘Pick’s disease’ for just one of the types of changes in the brain tissue that may be seen with the disease.
FTD is classically subdivided into two types:
- Behavioural variant FTD (bvFTD)
- Primary progressive aphasia (PPA), which includes progressive nonfluent aphasia (PNFA), semantic dementia (SD) and logopenic aphasia (LPA)
What causes FTD?
FTD is caused by loss of brain cells in the frontal and temporal lobes of the brain. However, the processes that lead to the loss of these brain cells are not well understood. There are a number of different underlying pathological changes that are recognised and several different pathological varieties of FTD. It is known that there is an abnormal accumulation in the brain cells of certain proteins (these include the proteins known as ‘TDP-43’, ‘FUS’ and ‘Tau’) but we do not yet fully understand why this accumulation occurs, or how it leads to the loss of cells.
In somewhere between 30 and 50% of cases a person with the disease may have a family history of the disease in one of their parents, brothers or sisters. In these cases the cause is more likely to be genetic. Problems in the tau (or MAPT) gene, progranulin (or GRN) gene or a gene called C9ORF72 are the cause in some of these cases, but not all abnormal genes have been discovered yet. Genetic testing is available in some centres. Other genes known as VCP, TARDBP, FUS and CHMP2B are extremely rare causes of FTD. Testing for these is not generally clinically available.
Links to other diseases
In a small number of patients FTD can overlap with one of a number of diseases that affect movement of the body: motor neurone disease (MND, sometimes called amyotrophic lateral sclerosis, ALS), progressive supranuclear palsy (PSP) or corticobasal degeneration (CBD). Symptoms of MND can include weakness of the limbs or problems with swallowing. PSP causes problems with movements of the eyes as well as problems with thinking and behaviour. There are often other physical problems such as falls, difficulty walking and stiffness. Some patients with FTD will later develop symptoms similar to Parkinson’s disease such as slowing of movements, tremor and stiffness of the limbs.
 Close
Close

