3D ‘bio-printing’ inside hydrogels could help understanding of how cancer spreads
9 June 2023
Scientists from across UCL, Great Ormond Street Hospital and the University of Padova have shown how 3D printing can be achieved inside ‘mini-organs’ growing in hydrogels, which could help better understand how cancer spreads through different tissues.
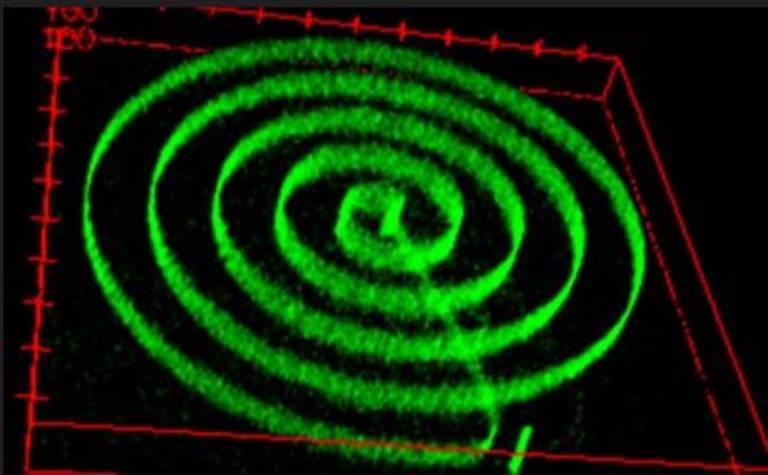
The new technique can help control the shape and activity of the mini-organs, and even force tissue to grow into ‘moulds’. The researchers hope that this will allow teams to produce realistic models of organs and disease, and study cells and organs more accurately.
Organoid science is a particularly promising area of research at the Zayed Centre for Research (a partnership between the UCL Great Ormond Street Institute for Child Health and Great Ormond Street Hospital). It involves the creation of micro-versions of organs such as the stomach, intestines and lungs.
However, the tissue almost always grows in an uncontrolled way and doesn’t represent the complex structure of naturally occurring organs. This is particularly important as an organ’s shape and structure is as crucial as its cellular makeup.
The new research, published in Nature Communications, shows for the first time how scientists can create solid structures within a pre-existing gel to solidify specific patterns in real time, guiding organoids growing in the gel into a particular structure by using light from a high-specification microscope. This means that any cell in the growing mini-organ or entire organoids will grow in a specific and precise way.
For example, to study how cancer travels through tissue of different hardness and density, the team created hardened gel cages around cancer cells and monitored how their movement changed depending on the density of its surroundings – this is important for understanding the spread of cancer.
By creating better models of disease, future studies will be more reliable and have better quality results. Researchers hope this will eventually lead to a reduction in animal research.
The team now plan to use the technique to recreate and study what happens to an organ’s function when it doesn’t grow correctly – for example in many malformations that develop in the early stages of pregnancy.
The work could also lead to treatment through the delivery of biologically accurate ‘patches’ in living organs.
Co-lead author of the research, Dr Giovanni Giobbe (UCL Great Ormond Street of Child Health), said: “It’s been amazing to see these precise structures begin to form before our eyes due to our small but painstaking adjustments in the polymer gel.
“We’re really excited to see where this can take us in the understanding of human disease and one day, treatment.”
To explore the ‘printing’ uses of the technique the team applied the method to several different situations.
For example, to study neurons, organoid research would traditionally create disordered bundles of neurons that are impossible to isolate and study. However, this technique allows the team to create hardened gel ‘rails’ for the neurons to grow along, like the lanes of an Olympic pool.
Meanwhile, to ensure that microscopic intestines are created with the same shape as ‘real’ developing intestines, the team created a complex hydrogel mould that guided organoids into shapes that mimic the complex structure of a developing intestine called ‘crypts’ and ‘villi’.
Similarly, scientists were able to pattern a hydrogel to encourage lung cells to create branches, like they do in a real lung.
Professor Paolo De Coppi (UCL Great Ormond Street Institute of Child Health, paediatric surgeon at GOSH, and co-lead of the tissue and engineering and regenerative medicine theme at the NIHR GOSH BRC), said: “This work is an excellent example of how we can bring interdisciplinary, international teams together to improve our research and benefit patients.
“Teams at GOSH and UCL that specialise in organoid research in the UK, working with Italian teams specialising in design and application of gel-printing, are what have made this incredible and beautiful piece of research come to fruition. This will have implications for laboratory-based research to improve our understanding of disease but could also lead to in-patient uses and treatments.”
Next steps for this work will be to study these controlled, moulded and directed mini-organs to better understand how they can mimic real organs and conditions in the body.
Dr Anna Uriuolo (University of Padova and lead of the Neuromuscular Engineering Lab at the Institute of Paediatric Research) said: “This work in an exemplar of the advancements of the multidisciplinary approach that is exploding in biomedical research. The ability to reproduce models of organs in the lab and the development of technologies that help scientists to recapitulate healthy and diseased tissues and organ complexity on the bench is the outset of how translational medicine will change in the next future.”
This work was funded by 2017 STARS-WiC grant of University of Padova, Progetti di Eccellenza CaRiPaRo, TWINNING of University of Padova, Oak Foundation Award, AFM Telethon, ‘Consorzio per la Ricerca Sanitaria’ (CORIS) of the Veneto Region, Italy (LifeLab Program), European Research Council (ERC, RerOids) to N.E., and the STARS Starting Grant 2017 of University of Padova and IRP Consolidator Grant to A.U., NIHR GOSH Biomedical Research Centre and GOSH Children’s Charity.
Links
- Research in Nature Communications
- Dr Giovanni Giobbe's academic profile
- Professor Paolo De Coppi's academic profile
- UCL Great Ormond Street Institute of Child Health
- UCL Population Health Sciences
- NIHR GOSH BRC
Image
- Credit: Urciuolo and Giobbe et al
Media contact
Poppy Danby
E: p.danby [at] ucl.ac.uk
 Close
Close


