UCL severe acute malnutrition research published
22 July 2009
Links:
 thelancet.com/journals/lancet/article/PIIS0140-6736(09)60884-9/abstract" target="_self">Lancet PRONUT research paper summary
thelancet.com/journals/lancet/article/PIIS0140-6736(09)60884-9/abstract" target="_self">Lancet PRONUT research paper summary
UCL researchers have undertaken a study, published in The Lancet of 11 July, to ascertain whether the treatment of severe acute malnutrition could be improved through the use of new types of therapeutic foods.
UCL Centre for International Health & Development Research Fellow Dr Marko Kerac, together with Dr Andrew Seal, and honorary fellow Dr Steve Collins were part of the 'PRONUT' study team, which was led by Valid International UK and conducted in partnership with The College of Medicine, Malawi.
The project aimed to assess the clinical and nutritional efficacy of probiotics and prebiotics in the treatment of severe acute malnutrition in a setting where HIV is common. Probiotics are live bacteria, which are considered beneficial and not harmful. Prebiotics are non-digestible fibres which may work by stimulating the growth of 'good' bacteria in the intestines. When used together, they work to promote health and wellbeing over and above the provision of essential food nutrients.
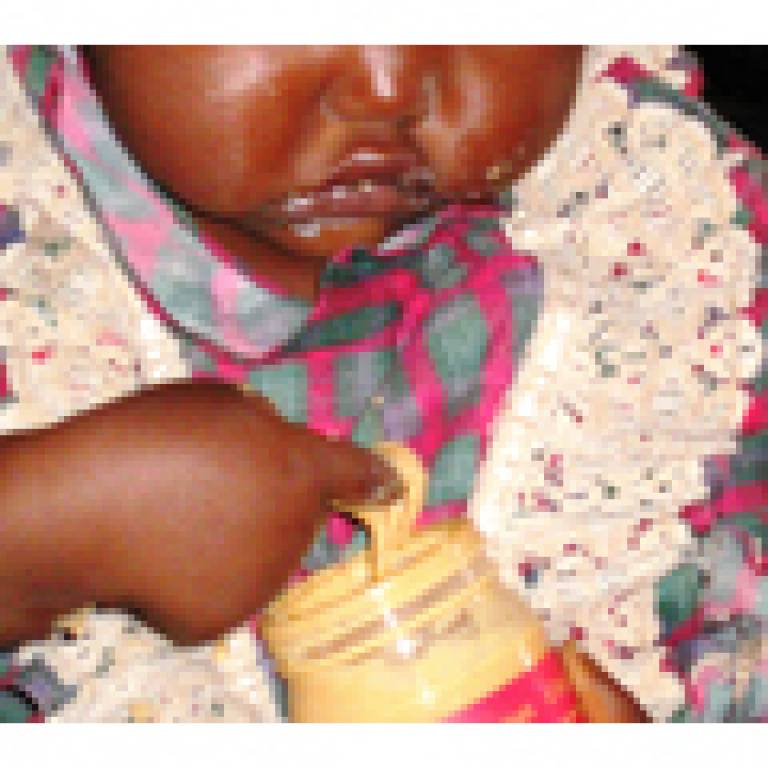
The study was conducted over a nine-month period at MOYO nutrition rehabilitation unit, Queen Elizabeth Central Hospital, Malawi and recruited 795 Malawian children aged between five months and 13 years old.
Probiotics were given for the duration of the treatment mixed into high-energy nutrient-dense 'Ready-to-Use Therapeutic Food', the standard diet for malnourished children. The study found that overall results were negative concluding that the probiotic/prebiotic mix does not improve treatment outcomes.
Lead author and principle investigator Dr Marko Kerac said: "Such negative results are important as positive findings: in a world of limited resources, it enables us to focus on those interventions that do work. In order to make an impact on global health priority conditions such as malnutrition, it is vital to ensure that existing treatments are being delivered well and are reaching all children affected. Only then will additional therapies have the best chance of making an impact."
Between 13 and 19 million children are affected by severe acute malnutrition globally. Each year over one million die from the condition. Most children with severe acute malnutrition live in south Asia and central Africa, where severe acute malnutrition accounts for a large number of deaths in children aged under five years old.
In the same issue of The Lancet, Drs Kerac, Seal and co-authors from Valid International and the Clinton Foundation USA, also described the implications of changes in the way malnutrition is diagnosed. New definitions are based on the World Health Organization (WHO) growth standards, an international gold standard describing how children should grow when measured by weight and height. To date there has been no documentation to show which definitions different countries are using. This means the numbers of children diagnosed as malnourished can vary greatly across different countries. In the article entitled 'New WHO growth standards: roll-out needs more resources' also published in the Lancet this month, they outline the main challenges ahead:
- Current treatment supply is already insufficient, with only nine per cent of children affected by severe acute malnutrition receiving treatment.
- Diagnosing malnutrition using the new criteria based on WHO growth standards will further increase the numbers of children eligible for treatment.
- To meet the increased treatment needs, substantial financial investment is necessary to create and sustain feeding programme expansion.
- Strategic rollout is essential for both feeding programmes and the new WHO growth standards: only when treatment supply is in place will it be possible to cope with the increased demands due to the new standards.
UCL context
Avoidable and preventable death and disease are among the major challenges facing the world today. At UCL we are in an excellent position to help overcome the barriers to global health when we work together.
The solutions to achieving this reside equally in all our disciplines: from the arts and humanities, built environment, engineering and law to basic and applied biomedical sciences.
UCL has prioritised the Grand Challenge of Global Health. The UCL Institute for Global Health is the hub bringing together UCL's immense multidisciplinary wealth of intellectual capital and international collaborations to provide innovative, workable solutions to global health at scale.
Related news
UCL Global Health Symposium - Fatal Neglect: Forgotten issues in child health
UCL at Commonwealth and WHO health meetings
 Close
Close

