Project Summary

Pneumonia remains the leading cause of infectious deaths amongst children under-five worldwide, with the highest burden seen in sub-Saharan Africa.
Malnutrition plays a key role in pneumonia morbidity and mortality in this setting. Therefore, early and accurate identification of children who are malnourished or have poorer cellular health could reduce mortality as these children could be referred into more intensive care. Not only could this reduce pneumonia-related mortality, but it could also have positive effects on community perceptions of healthcare, as children are treated appropriately and underlying malnutrition is highlighted.
Bioelectrical impedance analysis is a technology developed to predict physiological parameters from bio-electrical properties. It has been widely used to predict total body water and hence body composition, but requires population specific equations for this purpose. A more innovative approach involves 'bioelectrical impedance vector analysis' (BIVA), which allows hydration and body cell mass to be differentiated non-invasively. It can also be adapted for local or segmental application, in order to acquire bio-electrical data from specific body regions. The utility of BIVA to differentiate oedema and predict mortality in Ethiopian children with severe-acute malnutrition has recently been demonstrated.
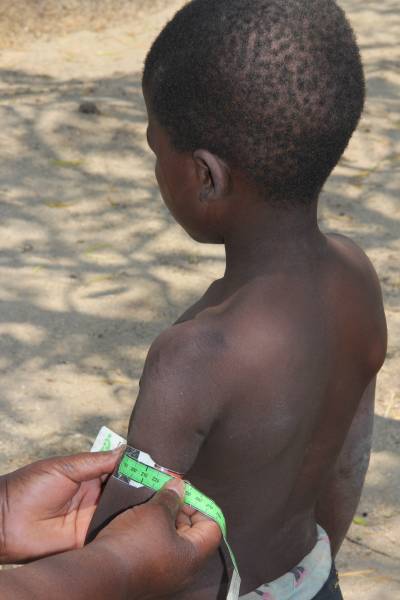
In this mixed-methods project we are assessing the feasibility of using BIVA to measure cellular health as an indicator of nutrition status in children diagnosed with pneumonia, in Malawi. We hypothesize that BIVA will give a more reliable and accurate measurement of nutritional status than the currently widespread measure of mid-upper arm circumference (MUAC). This offers a novel approach for improving the assessment of malnutrition in sick children, with the potential to be adapted into an integrated mHealth tool for both community health workers and facility staff.
 Close
Close

