START is a large-scale randomised controlled trial assessing the effectiveness of Multisystemic Therapy for reducing out-of-home placement and offending behaviour in young people in 9 sites across England, compared to management as usual. Data collection for the trial has concluded in Autumn 2017 and the results are currently in the process of being prepared for publication.
What is Multisystemic Therapy?
Multisystemic Therapy (MST) is an intervention specifically designed for young people who exhibit antisocial behaviour, and their families. The programme was original developed in the United States to help young people who were at higher risk of becoming young offenders. The strength of MST is in integrating different elements of treatment (such as cognitive-behavioural therapy and family therapy), and focusing on different aspects of the young person's environment, such as home life, school, friends, and the community. MST therapists work intensively with the young person to help them reduce anti-social behaviour, improve family relationships, tackle personal problems such as substance misuse, encourage positive activities, and give the parents or carers the tools to help them manage the young person's behaviour.
Nine principles of Multisystemic Therapy
- Finding the Fit: The primary purpose of assessment is to understand the 'fit' between the identified problems and their broader systemic context.
- Positive and Strength Focused: Therapeutic contacts should emphasise the positive and should use systemic strengths as levers for change.
- Increasing Responsibility: interventions should be designed to promote responsibility and decrease irresponsible behaviour among family members
- Present- focused, Action-orientated and Well-defined: intervention should be present-focused and action-orientated, targeting specific and well-defined problems.
- Targeting Sequences: intervention should target sequences of behaviour within and between multiple systems that maintain identified problems.
- Developmentally Appropriate: interventions should be developmentally appropriate and fit the developmental needs of the youth.
- Continuous Effort: interventions should be designed to require daily or weekly effort by family members.
- Evaluation and Accountability: interventions efficacy is evaluated continuously from multiple perspectives, with providers assuming accountability for overcoming barriers to successful outcomes.
- Generalisation: interventions should be designed to promote treatment generalisation and long term maintenance of therapeutic change by empowering caregivers to address family members' needs across multiple systemic contexts.
What is the START trial?
Although evidence from the US suggests that MST is a very promising treatment for young people with antisocial behaviour problems, it has not yet been fully explored in a UK context. The Systemic Therapy for At-Risk Teens (START) trial was started in 2009 as a randomised controlled trial with the aim of comparing the outcomes of MST with management as usual (MAU), i.e., the services and support which this group of young people would typically receive in its absence.
The primary aim of the study was to determine whether MST was more effective than MAU at reducing the risk of young people being placed into out of home care because of antisocial behaviour, mental health problems, or other unmet needs. Secondary aims also included assessing whether MST was more effective than MAU at improving family functioning, educational outcomes, mental health and behavioural problems. The trial also included an economic analysis to determine the cost effectiveness of MST compared to MAU.
The trial was initially scheduled to collect data from baseline (when the family was first recruited into the trial) to 18 month follow-up. This phase was termed START I. However, the trial was then extended to a 5-year follow-up, for a phase termed START II.
Who took part?
|
Sites:
|
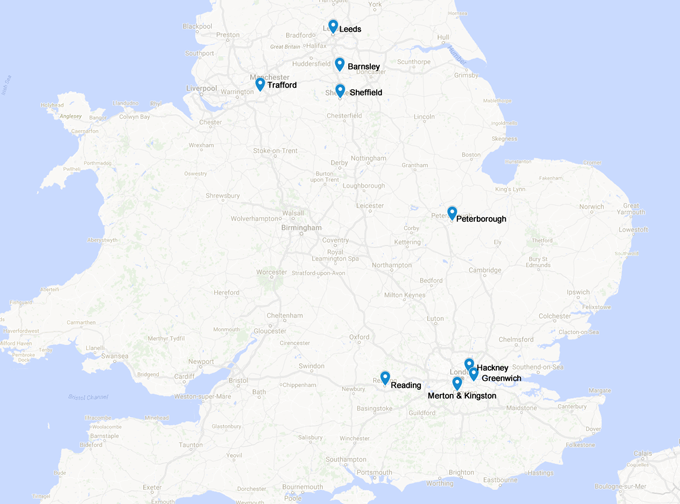 |
In total, 685 young people and their carers were recruited into the trial from 9 sites, with 50% randomly allocated to the MST and 50% to MAU. Young people were referred to the trial through social services, Child and Adolescent Mental Health Services (CAMHS), and youth offending services. The young people were aged between 11 and 17 years, and were only accepted into the trial if they met specific referral criteria, including a past history of conduct problems, history or risk of offending, and sufficient family involvement for the programme to be suitable (a full list of inclusion and exclusion criteria can be found in the protocol paper, linked below).
Families which received MST worked with a specially trained MST therapist for an intensive period of 3 to 6 months (depending on family needs). Families who were randomised into the MAU arm received standard care offered by social services to young people with these types of problems. Typically, this would mean involvement from different services depending on the young person's specific needs, such as CAMHS, or a specialist substance misuse service.
How was data collected?
If referral was successful and the young person met all inclusion criteria, the family was invited to take part in the trial. Participation was entirely voluntary and all participants were asked to sign consent forms agreeing to take part.
Researchers from the trial initially met with the young person and their carers at baseline (when they were first recruited into the trial). Data was collected again at 6 months, 12 months, and 18 months for START I. At each time point, researchers asked the young people and their carers to complete a series of questionnaires, designed to cover a wide range of measures of functioning and well-being.
When the trial was extended to 5 years (START II), data was also collected at 24, 36, and 48 months. Additional data collected from external databases (offending and school participation) up to 60 months.
For a full list of questionnaires and the constructs they measure, see: http://www.isrctn.com/ISRCTN77132214
What were the findings?
The results of START I (baseline to 18 months) are being prepared for publication in a peer-reviewed journal, and are due to be available in late 2017. The results of START II (18 to 60 months) are currently in the analysis stage and should be available in 2018.
Funders
START I: Department for Children, Schools and Families (now the Department for Education) in conjunction with the Department of Health (UK)
START II: NIHR Health Services and Delivery Research Programme
Chief investigator: Professor Peter Fonagy
Trial team:
Dr Stephen Butler
Prof Sarah Byford
Prof David Cottrell
Prof Peter Fuggle
Prof Ian Goodyer
Prof Freidrich Lösel
Prof Stephen Pilling
Prof Stephen Scott
Dr James Wason
Dr Ian White
Dr Helene Joffe
Dr Alisa Anokhina
Rachel Haley
Elizabeth Simes
Contact
For information about the trial, please contact the Trial Coordinator. alisa.anokhina@ucl.ac.uk
Useful links
1. Protocol
Fonagy P, Butler S, Goodyer I, Cottrell D, Scott S, Pilling S, Eisler I, Fuggle P, Kraam A, Byford S, Wason J, Haley R, Evaluation of multisystemic therapy pilot services in the Systemic Therapy for At Risk Teens (START) trial: study protocol for a randomised controlled trial., Trials, 2013, 14, 265, doi: 10.1186/1745-6215-14-265.
PubMed abstract: https://www.ncbi.nlm.nih.gov/pubmed/23962220
Publisher full text: https://trialsjournal.biomedcentral.com/articles/10.1186/1745-6215-14-265
2. ISRCTN record of the trial: http://www.isrctn.com/ISRCTN77132214
3. MST-UK website: http://www.mstuk.org/
|
|
 Close
Close

