Non-Ketotic Hyperglycinemia and the Glycine Cleavage System
Non-ketotic hyperglycinemia (NKH), or glycine encephalopathy, is a rare, life-limiting inherited metabolic disease characterised by accumulation of excess glycine in the body. The disease becomes apparent soon after birth with lethargy, breathing difficulties and neurological symptoms, including seizures. Affected infants suffer epilepsy and profound delay in development and NKH is often fatal in early childhood.
NKH is an autosomal recessive disease, in which one copy of the affected gene is inherited from each parent. Classic NKH is caused by mutations in GLDC or AMT, genes that encode components of the glycine cleavage system). The majority of children carry mutations in GLDC (glycine decarboxylase) and a broad spectrum of mutations have been identified.
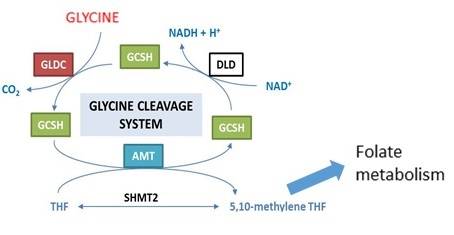
The Glycine Cleavage System (GCS) regulates the abundance of glycine by breaking it down in a reaction localised in mitochondria (Figure 1). Glycine is the smallest amino acid and functions both as a neurotransmitter in the central nervous system and as a precursor in a number of biosynthetic processes including production of proteins and purines (for DNA synthesis). The harmful effects of excess glycine in NKH are thought to result, at least in part, through the action at NMDA and glycine receptors in the CNS.
Current treatment for NKH is based on use of sodium benzoate, to lower glycine levels in the body, and management of epilepsy. These treatments do not provide a cure.
Mechanisms of neurulation and NTDs
Our research aims to determine the mechanisms of neural tube closure at genetic, molecular, cellular, tissue and whole embryo levels of organisation. In parallel, we are investigating a number of mouse models of NTD, to determine which aspects of the neural tube closure fails in each case.
This work can illuminate the normal embryonic process of neurulation, which is often considered a paradigm for morphogenesis in developing organisms. It also offers insight into the ways in which neurulation can become disturbed leading to clinically important NTDs, including spina bifida and anencephaly. By understanding how neurulation can be disturbed, we will be in a better position to develop new therapies to prevent human NTDs.
Planar cell polarity genes and neurulation
The planar cell polarity (PCP) pathway is a non-canonical Wnt signalling cascade that plays a key role in vertebrate embryonic morphogenesis. We provided the first evidence for a link between PCP and neurulation in mammals.
The PONTI study: inositol and prevention of NTDs
Some cases of NTD can be prevented by supplementation with folic acid before and during early pregnancy, but it is increasingly apparent that a significant proportion of NTDs fail to respond to FA. Most programmes of voluntary supplementation and folic acid food-fortification have observed a reduction in NTD prevalence of less than 50%.
As a result, NTDs continue to occur at an average frequency of 0.5-1.0 per 1000 established pregnancies, worldwide. We have explored the possibility that inositol, a vitamin-like molecule with a key role in cellular metabolism, has a NTD-preventive action that is independent of folic acid. If confirmed, this could lead to a combined approach to primary prevention of NTDs, involving both folic acid and inositol supplements.
Folate one-carbon metabolism and neural development
Folate one-carbon metabolism (FOCM) comprises a set of cellular reactions that transfer one-carbon units for a number of downstream functions including nucleotide biosynthesis and methylation reactions. Use of supplemental folic acid (the synthetic form of folate) before and during early pregnancy can prevent NTDs and all women planning pregnancy are recommended to take a folic acid supplement. These findings implicate folate metabolism in neural tube closure and a major focus of our research is to understand the relationship between folate status and susceptibility to NTDs.
 Close
Close










