Protein responsible for 'bad' blood vessel growth discovered
18 July 2013
The discovery of a protein that encourages blood vessel growth, and especially 'bad' blood vessels - the kind that characterise diseases as diverse as cancer, age-related macular degeneration and rheumatoid arthritis - has been reported in the journal Nature.
The team at the UCL Institute of Ophthalmology discovered the new protein, called LRG1, by screening for mouse genes that are over-expressed in abnormal retinal blood vessels in diseased eyes.
In these diseased retinas the LRG1 protein is expressed by blood vessel endothelial cells, which line blood vessel walls. LRG1 is also present in the eyes of patients with proliferative diabetic retinopathy - a vascular complication of diabetes that can lead to blindness.
The study shows that, in mouse models, LRG1 promotes the growth of blood vessels in a process known as 'angiogenesis'. Conversely, inhibition of LRG1 in mouse models reduces the harmful blood vessel growth associated with retinal disease.
The authors of the study suggest that blocking LRG1's activity is a promising target for future therapy.
Professor John Greenwood, senior author of the research from the UCL Institute of Ophthalmology said: "We have discovered that a secreted protein, LRG1, promotes new blood vessel growth and its inhibition prevents pathological blood vessel growth in ocular disease.
"Our findings suggest that LRG1 has less of a role in normal blood vessel growth and so may be particularly applicable to 'bad' blood vessel growth. This makes LRG1 an especially attractive target for therapeutic intervention in conditions where vessel growth contributes to disease."
Angiogenesis is an essential biological process that is required for development, reproduction and the repair of damaged tissues. However angiogenesis also plays a major role in many diseases where new vessel growth can be harmful.
For example, in the retina uncontrolled and irregular blood vessel growth in diseases such as age-related macular degeneration and diabetic retinopathy can result in a catastrophic loss of vision. Another example is the growth of cancerous solid tumours, which are dependent on the proliferation of new blood vessels. Angiogenesis is also an important feature of rheumatoid arthritis, where it contributes to the inflammation of the joint.
In
previous studies, many signalling molecules have been identified that control
angiogenesis, with the secreted protein vascular endothelial growth factor
(VEGF) being considered as the master regulator. Therapeutic targeting of VEGF
has resulted in improved outcomes in eye diseases with vascular complications
and in some cancers but it is clear that additional therapeutic targets need to
be identified.
Our findings suggest that LRG1 has less of a role in normal blood vessel growth and so may be particularly applicable to 'bad' blood vessel growth. This makes LRG1 an especially attractive target for therapeutic intervention in conditions where vessel growth contributes to disease.
Professor John Greenwood (UCL Institute of Ophthalmology)
The mechanism through which LRG1 promotes angiogenesis is by modifying the signalling of a multifunctional secreted growth factor called transforming growth factor beta (TGF-beta). TGF-beta regulates both the maintenance of normal healthy blood vessels, and the unwanted growth of harmful blood vessels, but precisely how it promotes two opposing outcomes is a biological paradox.
This study indicates that in the retinal diseases investigated LRG1 production is 'turned on' in blood vessels. This causes a switch in TGF-beta signalling away from a normal vessel maintenance pathway towards a pathway that promotes the growth of new harmful blood vessels.
Professor Stephen Moss, senior author from the UCL Institute of Ophthalmology said: "Genetic studies have revealed that the gene that codes for LRG1 is conserved in vertebrates, and this study confirms that mouse and human blood vessels express LRG1.
"We predict, therefore, that abnormal blood vessel growth is also a conserved process and that the role of LRG1 is equally applicable to human pathological angiogenesis."
He added: "Work is already underway to develop a therapeutic antibody that targets LRG1."
The research was funded by the Medical Research Council, the Lowy Medical Research Foundation, UCL Business, the Rosetrees Trust, the National Institute for Health Research (NIHR) Biomedical Research Centre at Moorfields Eye Hospital and UCL Institute of Ophthalmology (who are advising on the translational pathway) and the British Heart Foundation.
The discovery of a protein that encourages blood vessel growth, and especially 'bad' blood vessels - the kind that characterise diseases as diverse as cancer, age-related macular degeneration and rheumatoid arthritis - has been reported in the journal Nature.
Media contact: Clare Ryan
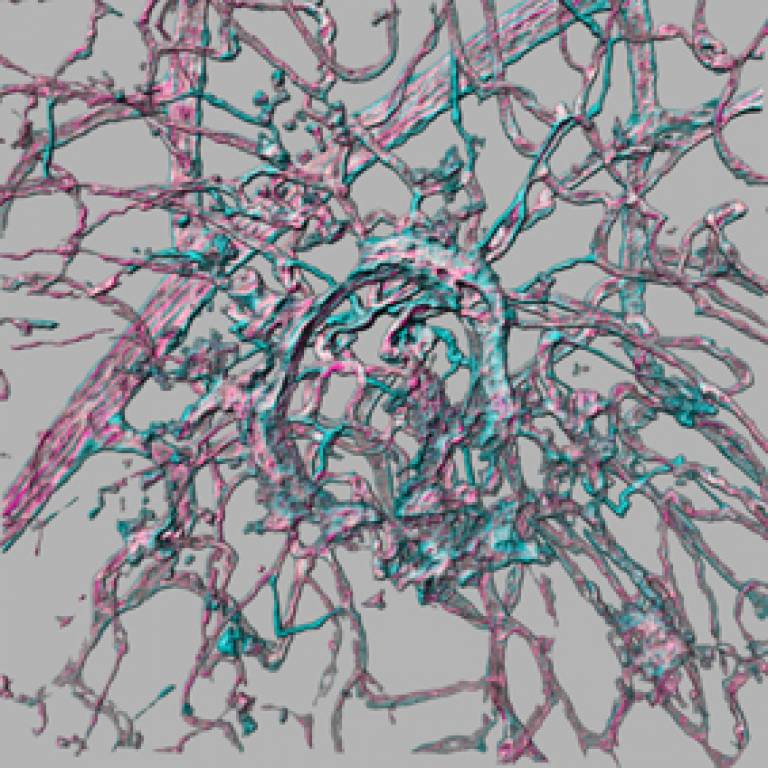
Image: Three dimensional reconstruction of blood vessels stained for the endothelial cell protein PECAM-1 (pseudocoloured magenta) and collagen IV (pseudocoloured cyan) showing a choroidal neovascular lesion and surrounding retinal vessels.
Links:
UCL Institute of Ophthalmology
Research article in Nature (£)
 Close
Close

