FORECEE

Overview
The FORECEE project is focused on the implementation of omics based methods into wide scale clinical practice for the stratification and risk prediction of cancers that are hormone-associated and specific to women (breast, ovarian, endometrial and cervical cancers). These represent more than 47% of all cancers in women and amongst them are cancers with a 5-year survival rate of less than 40%.
This project originates from cutting edge research, conducted by several members of this consortium, which has identified a novel and exciting opportunity to exploit omics methods in the prevention of female specific cancers.
A critical factor in the prevention of cancer is access to the cell of origin (Figure 1). Cervical screening, through application of the Papanicolaou test (or Pap smear) and/or human papilloma virus (HPV) testing assesses which women are at risk of developing an invasive cervical cancer and would benefit from a preventive procedure (ie excision of the cervical area at risk). Widespread introduction of the Pap test has reduced both the incidence of cervical cancer and associated deaths by up to 80%1. The accessibility of the cancer’s cell of origin from the uterine cervix and recognition of risk markers reflecting an individual’s interaction and response to environmental exposure, in this case to HPV, are integral to this success.
In sharp contrast, breast, endometrial and ovarian cancers continue to pose considerable challenges in terms of risk prediction. Access to the cell of origin for these cancers can only be achieved with fully invasive methods such as a random breast biopsy, a hysteroscopy and endometrial biopsy or a laparoscopy under general anaesthesia. These options are definitely not feasible for the general population and hence our ability up to date to stratify and identify high risk groups is severely restricted.
We posit that the epigenome is the ideal surrogate which records the individual response to environmental disease-triggering factors. The epigenome is known (1) to vary across tissues and (2) depend on sensors (i.e. hormone receptors) to record individual responses to cancer-promoting factors (i.e. a large component in all women’s cancer is aberrant exogenous and endogenous hormonal exposure). Cells from the uterine cervix are the only cell type which (i) is both epithelial (hence same cell type as the cell of origin for all four women specific cancers) and responsive to hormones and (ii) can be easily accessed. These cells can also be used to analyse the genetic component of the risk (i.e. analysis of single nucleotide polymorphisms) and microbial factors (HPV and vaginal microbiome) which contribute to the development of female genital tract cancers.
Hence we have identified the possibility of utilising cervical cells, which remain abundant in the clinical setting [97% of cells in a cervical liquid based cytology (LBC) sample are not required for the cervical cancer screen], combined with a multi-omics enabled analysis pipeline to provide a bridge for the prevention of all major female specific cancers (Figure 1). The FORECEE project is aligned with the novel concept of “P4 Medicine” (predictive, preventive, personalized, and participatory) seeking to develop a multi-omics enabled risk prediction tool and translate the tool’s output into recommendations for new clinical pathways for screening and prevention of all female cancers that can be implemented on a national/international scale. The multi-disciplinary FORECEE team present leading expertise in epigenetics, genetics, metagenomics, health economics, risk prediction, communication, Health Technology Assessment as well as population health and is uniquely placed to develop and specify the future strategy and policy for the prevention of female specific cancers.
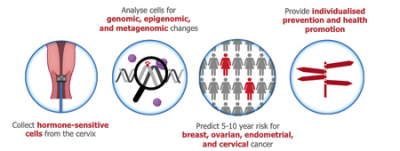
Figure 1. The FORECEE Vision – the use of cervical cells and omics-based analysis to predict the risk of all women specific cancers
Design
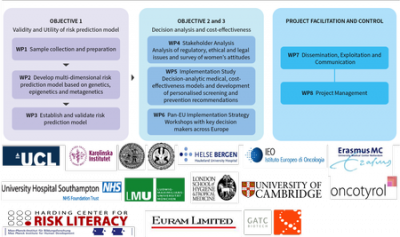
Key Hypothesis
Vital information about a person’s individual genetic / epigenetic risk of cancer may be acquired from a multi-cellular panel of alterations consisting of buccal, blood and/or cervical cells.
Principle Outcomes
1. Establishment of a biobank of buccal, blood and cervical cells from a range of research volunteers and patients with a view to establish a biobank containing biosamples that can be used for genomic (SNPs), epigenomic (methylomic) and microbiomic analysis.
2. Development of stratification algorithms and precision tools based on a systems biology assessment of the genetic/epigenetic/microbiomial data of the collected samples, to better predict risk of disease or mutation status. 3. Insight into the cell-autonomous and non cell-autonomous (systemic) factors that drive female cancer development with a view to aid stratification and individualise therapeutic and preventive strategies.
Planned Analyses
Samples will be investigated as described below. 1. Analysis of the genome (SNPs) elements that may inform risk prediction and individualise preventive strategies. 2. Analysis of the epigenome (principally DNA methylation changes) in various buccal, blood and cervical cells, as well as paraffin-embedded tissue.
- Analyses of the microbiome (16s RNA locus) in cervical/vaginal swabs.
- Epidemiological and health behaviour assessment of different groups of
participants at different times (pre- and post-genetic testing etc).
Recruitment
We will recruit study participants in clinics, by invitation and by public adverts.
Following appropriate time for question and reflection, appropriate consent will be obtained. Participants will be allocated a unique volunteer reference number. Information collected will include patient details e.g. name, address, NHS number, GP details, demographic information and summary of family history of breast, ovarian and other cancers and any epidemiological data relevant to the project.
We aim to recruit women aged 18-75 years in the following groups:
- Women with current ovarian, especially High Grade Serous Ovarian, Endometroid, Mucinous, or Clear Cell types.
- Women with current endometrial cancer, especially poor prognostic cancers such as Grade 3, Clear Cell or with Serous histology.
- Women with current breast cancer, especially any with Grade 3 and/or node-positive and/or ER/PR-negative and/or T2 and above
- Women with first presentation with abnormal smear (CIN3+)
- BRCA1/2mut or Lynch Syndrome mutation carriers
- Women with benign gynaecological conditions
Healthy volunteers from the general population
All participants will be provided with a detailed participant information sheet to help them make an informed decision regarding participating in the study. It covers issues pertaining to the implications of participating in the study, the advantages and disadvantages, sources of independent information and contact details for the study team. Participation will be completely voluntary and under no circumstances impact any clinical care received. The participant information sheet is attached to this application.
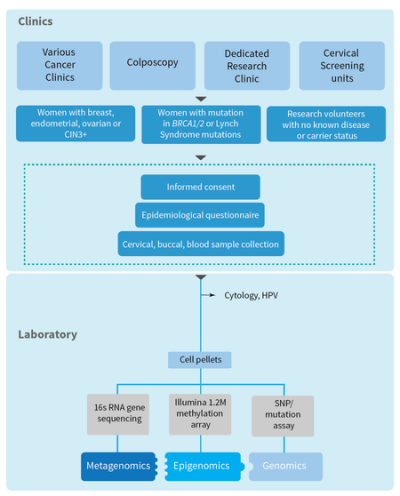
Workflow overview indicating the key stages of recruitment and data entry.
Team

The FORECEE Consortium gathered for the first time during the project at University College London in September 2015. With an excellent attendance of 34 representatives from 13 participating organisations, funders (EU and The Eve Appeal), and patient representatives, the kick off meeting gave each project partner the opportunity to introduce themselves to the group and to describe their role over the four years of development to come.
Clinical Collaborators
Barts and the London (Dr Ranjit Manchanda)
Royal Free Hsopital (Prof Mo Keshtgar)
Imperial College London (Dr Maria Kyrgios)
Great Ormond Street Hospital (Dr Lucy Side)
Southampton University Hospital (Dr Richard Hadwin)
Charles University Prague (CU)
European Institute of Oncology (IEO)
Ludwig Maximilian University (LMU) Haukeland University Hospital Bergen (HBE)
Research Team
Prof Martin Widschwendter (Principal Investigator)
Dr Dan Reisel (Study Coordinator, Recruitment)
Miss Allison Jones (Scientific Coordinator, Sample Processing)
Dr Iona Evans (Scientist)
Dr Kantaraja Chindera (Scientist)
Dr Susanne Knapp (Research Associate)
Funding
The Eve Appeal
The Eve Appeal is a registered charity, formed in 2005. Since then, they have worked hard to raise money to fund the world-class research programme at the Department of Women's Cancer based at University College London (UCL).
The Department's vital and much-needed research will benefit women in the UK and worldwide.
Eve Appeal www.eveappeal.org.uk/
Horizon 2020
The EU Framework Programme for Research and Innovation. Following a very competitive call, the FORECEE Study was successful and received 8M Euro from the Horizon 2020 programme.
Horizon 2020: https://ec.europa.eu/programmes/horizon2020/
 Close
Close

