Tuberculosis
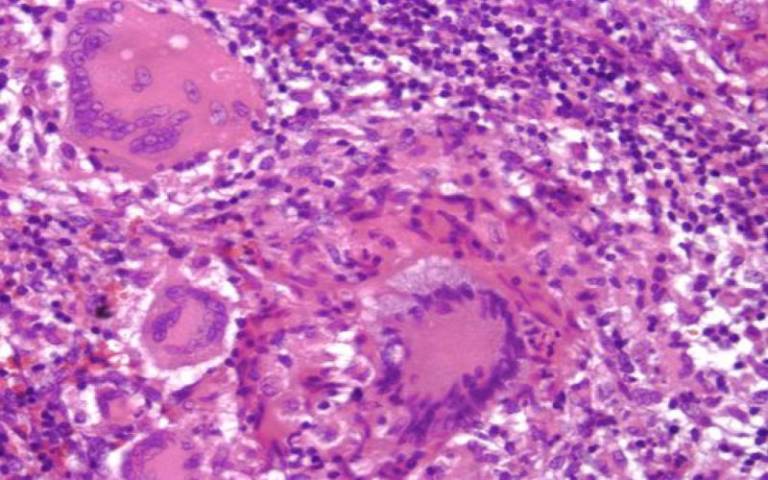
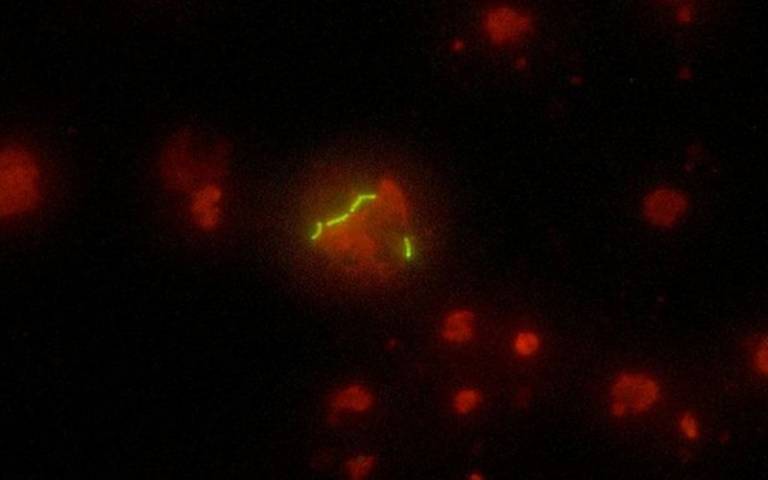
The main microscopic feature in specimens from the site of disease is the presence of granuloma- representing a focus of chronic inflammation with macrophages, neutrophils and T cells-often associated with cell death in a pattern called caseous necrosis. Consequently attention has focussed cellular immune responses to infection.
Assessments based on the presence of T cell immune memory for mycobacterial antigens suggest that substantial proportions of the global population have experienced infection but the vast majority of these people never experience disease. Importantly, disease can manifest in people for long periods of time after they migrate from communities with a high incidence of infection to one with very low incidence, suggesting that infection can remain sub-clinical or latent for many years. In the general population there is a 10% life time risk of disease amongst those who have some evidence of prior infection.
The most important risk factors for the development of TB disease are inherited immunodeficiencies, HIV co-infection and AIDS and other factors that may be expected to compromise immune responses, such as anti-TNF therapies, ageing, vitamin D deficiency, corticosteroid treatment and diabetes. Taken together, these observations suggest that human immune responses successfully protect against active disease in most people who have become infected, hence we focus on trying to understand how the immune system protects against TB disease.
A significant body of data suggests that Mtb can survive and replicate inside macrophages. Therefore we study innate immune host-pathogen interactions during infection of human monocyte derived macrophages with Mtb, and the capacity of macrophages to control mycobacterial growth with and without T cell help.
In addition we use transcriptional profiling at the site of tuberculin skin tests as a standardised mycobacterial challenge to characterise in vivo human immune responses to Mtb with molecular and systems level resolution. We use these experimental strategies to test the effect of HIV-1 co-infection, anti-TNF therapy, vitamin D deficiency and to identify immunological correlates of protection or disease.
Major challenges in TB research
- We don't understand how the immune system protects against TB.
- We can't distinguish persistent (or latent) infection from infection which has been cleared.
Our objectives
- Identify immunological correlates of protection in order to inform rationale designs of new vaccines, and to develop host-directed therapies for active TB to be used in combination with antimicrobial drugs, in order to significantly reduce the duration of treatment, reduce severity of disease and mitigate against the risks of antimicrobial resistance.
- Identify the immunological correlates of disease which stratify the risks of active disease in exposed individuals, in order to treat asymptomatic infection before it progresses to active TB.
 Close
Close

