
Project Summary
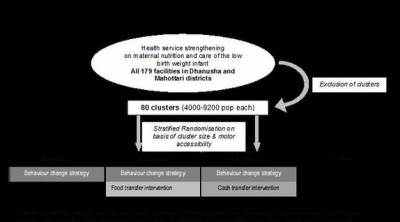
This cluster randomised controlled trial (cRCT) is assessing the relative impacts on birth weight of an nutrition behaviour change strategy (BCS), with and without an unconditional cash transfer or a food supplement, compared with current programmes, in two districts in southern Nepal. The study is powered to detect a 50 g difference in birth weight between allocation groups: BCS, BCS plus cash, BCS plus food, and control.
The behaviour change strategy uses a women's group participatory learning and action cycle combined with home visits to pregnant women, particularly those not attending groups. The groups discuss the problem of low birth weight, its causes and how to improve poor maternal nutrition. They then prioritise problems / causes that they feel are most important in their community and implement strategies to address them. Often these strategies involve awareness raising campaigns playing picture card games with groups of community members or conducting street dramas.
The monthly cash transfer is NPR 750, or NPR 5250 per pregnancy over which a woman receives 7 transfers. The food transfer, supplied by the World Food Programme, is a monthly 10 Kg ration of a fortified wheat-soya blend with 10% sugar, called "Super Cereal". This contains macro- and micro-nutrients needed in pregnancy and has been field tested and is acceptable in Nepal.
The primary outcome is birth weight measured on infant scales accurate to 10 g. Secondary outcomes include prevalence of low birth weight (% < 2500 g), maternal weight gain during pregnancy, preterm delivery, miscarriages, stillbirths, neonatal mortality, maternal and newborn illness, maternal eating behaviour, exposure to women's groups for pregnant women and family members, access to food transfers and cash transfers, and intra-household food allocation.
We are collecting data for at least 3250 infants per arm - 13000 infants in total - enrolled and exiting over 22 months. The richness of the data will allow us to measure not only the outcomes of interest, but also to model the mediating mechanisms that generate such outcomes.
The programme team brings together MIRA, Nepal's leading health research organisation, with 20 years' experience of trials in poor populations; University College London Institute for Global Health, with world-class expertise in perinatal care, nutrition, women's development and the cost-effectiveness of community-based interventions; Save the Children, with 40 years' experience of pro-poor interventions and scale-up in Nepal; the World Food Programme's global experience in food supplementation and dietary analysis; and Institute for Fiscal studies experience of economics of cash transfers and their effects on nutrition.
The team emphasises value for money, clearly delineated contributions from each partner, a partnership ideology that emphasises Nepalese leadership, strong technical support in all the required domains, and mature links with the Government of Nepal and relevant institutions.
If the findings of the trial in Phase 1 warrant scale-up, Phase 2 may assess whether a new intervention can be delivered at acceptable cost-effectiveness under normal operating conditions, including in challenging environments.
 Close
Close

